
Our Review Process
Our articles undergo extensive medical review by board-certified practitioners to confirm that all factual inferences with respect to medical conditions, symptoms, treatments, and protocols are legitimate, canonical, and adhere to current guidelines and the latest discoveries. Read more.
Our Editorial Team
Shifa Fatima, MSc.
Author
Dr. Apoorva T, MHM.
MEDICAL ADVISOR
What is Diabetic Neuropathy
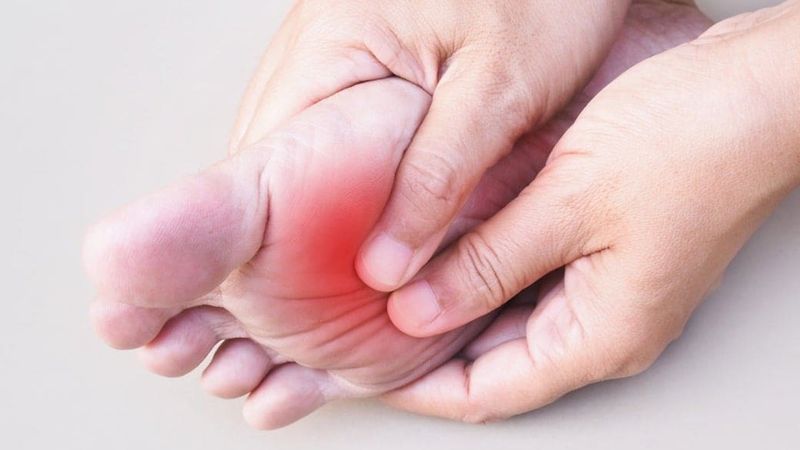
Neuropathy is a common complication of diabetes. Diabetes neuropathy is a complication of diabetes that affects the nerves. It can cause tingling, numbness, pain, and weakness in the feet and legs. Neuropathy can also impact the digestive system, heart, and sex organs. It can make it hard to walk, climb stairs, or do other everyday activities. Neuropathy can also lead to skin ulcers, which can become infected. It may occur in more than half of people with diabetes who have had the disease for ten years or more.
Neuropathy can cause significant disability if not taken care of at the right time. Let’s discuss how long does diabetic neuropathy take to develop and how to control diabetic neuropathy.
Table of Contents
Causes of Diabetic Neuropathy
There are many potential causes of neuropathy, some of which are reversible and some of which are not. Many cases of neuropathy are caused by damage to the nerves, which can be the result of several different conditions. Some common causes of nerve damage that can lead to neuropathy include:
- Diabetes: approximately 60-70% of people with high blood sugar levels develop some form of neuropathy.
- Alcoholism or drug abuse: People who drink heavily are at risk for developing neuropathy.
- Infections: Certain infections can cause nerve damage.
- Trauma: Injury to the nerves can lead to neuropathy.
- Vitamin deficiencies
- Autoimmune diseases
Types of diabetes neuropathy
There are four main types of diabetes neuropathy: peripheral, autonomic, proximal, and mononeuropathy.
Peripheral neuropathy
Peripheral neuropathy is a condition that results when the nerves that carry messages to and from the brain and spinal cord are damaged. This damage can disrupt the communication between the brain and the rest of the body, leading to various symptoms. Peripheral neuropathy is one of the most common types of diabetic neuropathy, and it impacts the nerves in your limbs.
Cures for peripheral neuropathy are not known, but there are various ways and treatments that can help lessen these symptoms. Some people with peripheral neuropathy need to make lifestyle changes to manage their condition.
You must consult a doctor if any one of the following symptoms of peripheral neuropathy is experienced by you, including:
- Tingling or numbness in the hands or feet
- Burning, prickling, or itching sensations
- Sharp, jabbing, or electric-shock-like pain
- Loss of muscle control and coordination
- Trouble balancing and walking
- Dry mouth and eyes
- Sexual dysfunction
- Constipation or diarrhoea
Autonomic neuropathy
Autonomic neuropathy is a disorder that results from damage to the autonomic nervous system. It controls all the body's "automatic" functions, such as digestion, blood pressure, bladder control, and heart rate. Damage to the autonomic nervous system can cause problems with these functions. It can cause constipation, diarrhoea, low blood pressure, and erectile dysfunction.
Proximal neuropathy
Proximal neuropathy is a type of peripheral neuropathy that impacts the muscles closest to the trunk of the body. It is caused by damage to the nerves that supply these muscles. This can lead to difficulty walking, climbing stairs, and other activities that require coordinated movement.
Symptoms of proximal neuropathy include weakness, pain, and cramping in the affected muscles. This is when you need lifestyle changes and consultation with the doctor to help manage symptoms and know how to treat diabetic neuropathy naturally.
There are several possible causes of proximal neuropathy, including injury, infection, and certain diseases. The condition may progress over time, leading to permanent disability. There is no cure for proximal neuropathy, but treatment depends on the underlying cause of the neuropathy. In some cases, treatment helps relieve symptoms and improve quality of life or may involve surgery or medication. In other cases, lifestyle changes may be necessary to help manage symptoms.
Mononeuropathy
Mononeuropathy (or mononeuritis) is a medical condition that affects just one nerve in the body. The most common type of mononeuropathy is carpal tunnel syndrome, which impacts the median nerve in the arm. Other types of mononeuropathy include radial nerve palsy, lumbosacral plexopathy, and peroneal nerve palsy.
Mononeuropathy can cause a wide range of symptoms, depending on which nerve is impacted. These can include pain, numbness, tingling, weakness, paralysis, and problems with movement or numbness in the hand and arm.
The condition can be caused by several things, including:
- Trauma or injury to the nerve
- Infection, such as meningitis
- Diabetes
- Autoimmune diseases, such as Guillain-Barre syndrome
- Cancer
What are the symptoms of autonomic neuropathy?
When it is affected, it can lead to various symptoms, including the following, and it is an alarming time for getting in touch with the medical expert.
- Dizziness
- Fainting
- Fatigue
- Nausea
- Vomiting
- Diarrhoea
- Constipation
- Urinary problems
- Sexual problems
- Low blood pressure
- High blood pressure

Diagnosis of diabetes neuropathy
If you have diabetes and are experiencing symptoms of diabetes neuropathy, see your doctor. They can diagnose the condition and recommend treatment. The earlier diabetes neuropathy is diagnosed, the better the chances for successful treatment.
Several different tests can be used to diagnose diabetes neuropathy. One important blood test used to diagnose diabetic neuropathy is the haemoglobin A1c test. This test measures a person’s average blood sugar level over the past three months. It can help doctors determine if someone has diabetes and, if they do, how well it is being controlled.
Other tests that may be used include physical examination, blood tests, urine tests, and nerve conduction studies: filament tests, sensory testing, nerve conduction testing, muscle response testing, and autonomic testing.
- Filament test: It is also called sensory testing, wherein a soft nylon fibre (monofilament) is brushed over areas of the patient's skin and the test to check the sensitivity to touch. It checks how nerves respond to vibration and changes in the surrounding temperature.
- Electrodiagnostic tests: These tests use electrical impulses to measure the health of your nerves.
- Nerve conduction studies: This test measures the speed of electrical signals as they travel along your nerves.
- Biopsy: This is a test in which a small sample of tissue is removed from your body so that it can be examined under a microscope.
- Muscle response testing is also known as electromyography; it measures the response of nerves in arms and legs to electrical signals.
- Autonomic testing is a simple test when the heart rate is assessed to various changes like standing and deep breathing by placing electrodes on your chest. Also know about sugar in urine test.
What is the treatment for diabetic neuropathy?
There are many treatments for diabetic neuropathy. Treatment options vary depending on the type and severity of neuropathy. Some people with neuropathy may not require any treatment. Others may need medication, physical therapy, or surgery.
There is no one-size-fits-all treatment for diabetic neuropathy. Learn how to treat diabetic neuropathy naturally by changing diet and having a healthy diet, lifestyle habits, checking on your blood pressure, being active, and doing regular exercises to prevent neuropathy from developing.
The objective of treatment is to maintain
- A slow progression of the disease is achieved by continuously checking the blood sugar levels to delay or prevent nerve damage.
- Relieving pain is advised through the prescribed meditation.
Manage complications and restore the function of the different organs by consulting separate specialists to prevent complications further.
Bottomline
This article covers the details of diabetic neuropathy and its reasons. There are mainly three neuropathies types: Peripheral, Autonomic, and Proximal. Causes, symptoms, and diagnosis of this condition are discussed so that the options of treatment through medication, surgery, or naturally with changes in lifestyle are well understood.
FAQs
Can you get rid of diabetic neuropathy in your feet?
No, you can not get rid of diabetic neuropathy in your feet. Once the nerve walls get damaged, they can not get repaired by themselves. The body can’t naturally repair the nerve damage. The only option left is to slow its progress by managing blood sugar levels and opting for a healthy lifestyle.
What is the best treatment for diabetic foot care?
There is no known cure for diabetic neuropathy. The goal of any treatment is to slow its progression, relieve pain and manage complications. This can be done by maintaining target blood sugar levels and relieving pain through medication.
How do you stop diabetic nerve pain in your feet?
Various pain-reliever medications can stop the nerve pain in your feet. For this, you should consult a doctor to know which medicine will be the best in your case. The medications can include anti-seizure drugs or antidepressants, or a mixture of both.
How do you reverse diabetic foot neuropathy?
At present, there is no way to reverse foot neuropathy. As the body can not reverse the nerve damage naturally, the condition can not be reversed. However, scientists are working on possible treatment procedures.
Is walking good for peripheral neuropathy?
Yes, some lifestyle modifications and exercises can help ease peripheral neuropathy pain. For this, you can go for a walk three times a week. It will relieve pain, improve muscle strength, and control blood sugar levels.
What is a good foot soak for neuropathy?
The American Diabetes Association discourages foot soaks for diabetic patients. When your feet are wet and wrinkly, they are more prone to damage. Just wash your feet with lukewarm (not hot) water every day and keep them dry.
References
- https://www.webmd.com/diabetes/diabetes-neuropathy
Disclaimer
This website's content is provided only for educational reasons and is not meant to be a replacement for professional medical advice. Due to individual differences, the reader should contact their physician to decide whether the material is applicable to their case.
More by Shifa Fathima

अर्जुनरिष्ट: फायदे, खुराक, नुकसान | पढ़ें | Sugar.fit

मधुमेह के लिए मधुनाशिनी वटी: उपयोग, लाभ, खुराक और दुष्प्रभाव|

मधुमेह को नियंत्रित करें भारतीय आहार से





