
Our Review Process
Our articles undergo extensive medical review by board-certified practitioners to confirm that all factual inferences with respect to medical conditions, symptoms, treatments, and protocols are legitimate, canonical, and adhere to current guidelines and the latest discoveries. Read more.
Our Editorial Team
Shifa Fatima, MSc.
Author
Dr. Apoorva T, MHM.
MEDICAL ADVISOR
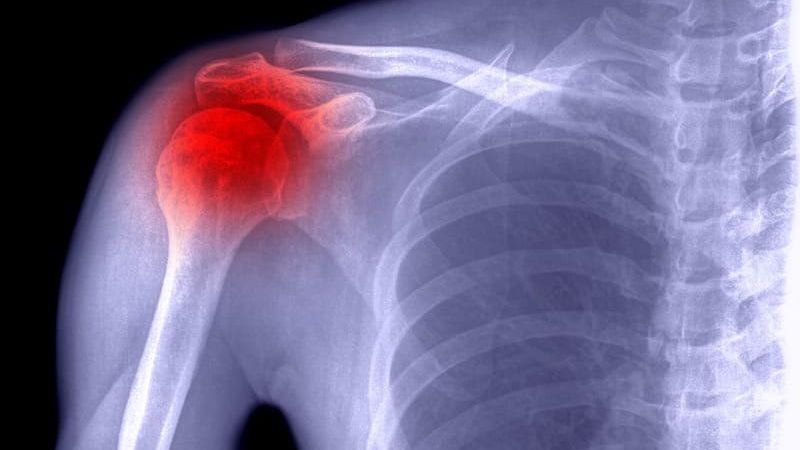
Frozen Shoulder and Diabetes
A frozen shoulder causes stiffness, pain, and decreased shoulder mobility. After the initial worsening of frozen shoulder symptoms, the condition usually improves, although complete recovery might take up to three years. If you suffer from a frozen shoulder, your doctor may recommend physical therapy sessions that increase your shoulder range of motion.
Table of Contents
What is Frozen Shoulder?
A frozen shoulder is a disorder that impacts the joint in the shoulder. It causes stiffness and pain that gradually worsens and then goes away. Your shoulder comprises three bones forming a ball-and-socket joint. The scapula, collarbone, and humerus make up your upper arm. The tissue holds everything together around your shoulder joint. We call this shoulder capsule.
Frozen shoulder happens when the capsule around the shoulder joint becomes tight and thick, making it hard to move the shoulder. Scar tissue bands form, and the amount of lubricating synovial fluid in the joint decreases.
What are the Causes of Frozen Shoulder?
1. Diabetes
Frozen shoulder is much more common in those who have diabetes. Diabetic patients with frozen shoulders also experience a greater degree of stiffness that lasts for a longer period before “thawing.”
2. Other health conditions
An overactive and underactive thyroid, heart disease, stroke, rotator cuff tear, and calcific tendonitis.
3. Recent surgery or injury
You may increase the risk of developing a frozen shoulder after a shoulder or arm surgery or injury if you keep your shoulder motionless for long periods.
4. Age and gender
Frozen shoulder is most frequent in people aged 40 to 60, and women are more prone to have it than men.
5. Altered arm mobility
During a hospital stay, do not move your shoulder for lengthy periods. The causes of frozen shoulder include excessive weight lifting and sudden stress due to injury.
What are the Symptoms of Frozen Shoulder?
- You may feel cramping pain in the shoulder
- Stiffness and discomfort make it difficult to move a frozen shoulder.
- The shoulder muscles around the top of the arm may also have pain.
- You may be having a similar sensation in your upper arm.
- You might find it difficult to get sleep at night due to worsening pain.

Who gets Frozen Shoulder?
Females are more likely to experience frozen shoulder than males, and the condition is most common between the ages of 40 and 60. The risk of developing a frozen shoulder is also higher in people with diabetes.
How is Frozen Shoulder related to Diabetes?
Collagen in the shoulder capsule can become sticky when sugar molecules bind to it, contributing to a frozen shoulder. Eventually, the changes to the collagen in the tendons and ligaments limit the range of motion. This occurs due to glycosylation, in which the glucose molecules attach to the protein molecules.
Frozen shoulder and diabetes have a connection because studies have reported that people with diabetes are at a higher risk for developing frozen shoulder than those who do not. It is due to their high blood sugar levels, which can cause problems in other parts of the body.
How to Diagnose Frozen Shoulder
Your doctor will examine you to diagnose a frozen shoulder. They will examine the pain level and range of motion. In the “active” part of the exam, you can move your shoulder yourself. They move it for you in the “passive” portion and note differences.
The doctor may give you a shoulder anesthetic. They will be able to more accurately evaluate your active and passive motion ranges with the help of this pain medication.
Your doctor may order an ultrasound, X-rays, or MRI to rule out other conditions that might cause discomfort and limit mobility, such as arthritis or a torn rotator cuff. Read more about diabetes causes.
Stages of Developing a Frozen Shoulder
Stage 1 : Freezing
Pain gradually increases during the “Freezing” stage. Your shoulder mobility decreases as the pain increases. The freezing stage can last from 6 to 9 months.
Stage 2 : Frozen
During this phase, you may experience reduced pain, but your stiffness will persist. Daily life may be highly challenging for four to six months during the frozen stage.
Stage 3 : Thawing
During “Thawing,” the shoulder motion increases slowly. It takes 6 months to 2 years to regain normal or near-normal motion and strength.
Treatment of Frozen Shoulder
1. Hot and cold compresses
This help alleviates swelling and pain.
2. Medication for reducing pain and swelling
These include acetaminophen and other non-steroidal anti-inflammatory drugs like ibuprofen to treat pain and inflammation. Your doctor may also recommend other pain relievers or anti-inflammatory medications. Steroid injections relieve pain and inflammation. Doctors inject corticosteroids into the shoulder joint. Also know about ayurvedic medicine for diabetes.
3. Transcutaneous electrical nerve stimulation
A small battery-operated device blocks nerve impulses and lowers pain.
4. Physical therapy
Stretching and range-of-motion focused physical session.
5. Home exercise
Continue exercise program at home.
6. Manipulation under anesthesia
Doctors will sedate you and force your shoulder to move during this procedure. It will cause the joint capsule to stretch, relieving the tightness.
7. Shoulder arthroscopy
The doctor will make an incision in the capsule surrounding your joint (capsular release). Doctors insert small instruments about the size of a pencil into incisions around the patient’s shoulder.
FAQs
How to Prevent getting a Frozen Shoulder
- Diabetics must check blood sugar levels regularly.
- Daily, stretch your back muscles and shoulder.
- You may strengthen your tendons by rotating your hands and palms to stretch various tendons.
- Use correct ergonomics while sitting at a desk and using a computer.
- Keep the immune system healthy.
- Beginning range-of-motion exercises soon after an injury or surgery is ideal.
What is the Main Cause of Frozen Shoulder?
Recovery from a shoulder injury, broken arm, or stroke can cause immobility, a risk factor for developing a frozen shoulder. Talk to your doctor about exercises you can do to keep your shoulder flexible if you've suffered an injury that limits your motion.
References
- https://diabetesstrong.com/frozen-shoulder-diabetes/
- https://www.diabetes.co.uk/diabetes-complications/frozen-shoulder.html
- https://my.clevelandclinic.org/health/diseases/15359-frozen-shoulder
- https://www.oamichigan.com/frozen-shoulder-syndrome-diagnosis-prevention-treatment/
Disclaimer
This website's content is provided only for educational reasons and is not meant to be a replacement for professional medical advice. Due to individual differences, the reader should contact their physician to decide whether the material is applicable to their case.








